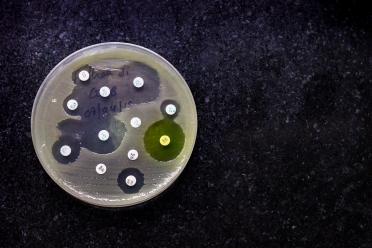
Before penicillin was discovered in 1928, bacterial diseases were wiping out populations - for example one sobering thought is that 90% of children that developed bacterial meningitis died, but the wide-scale production and deployment of antibiotics let us live without fear for the first time in human history.
Today, increasing numbers of people are dying from blood poisoning - sepsis is currently the largest killer of people in the world, and responsible for one in five deaths. Increasing AMR will only make this problem worse.
The use of antibiotics in food production is also a crucial issue for AMR. According to an assessment by researchers at the Chinese Academy of Sciences, China consumed nearly half the world’s antibiotics in 2013 — around 162,000 tonnes - just over half of which was administered to animals.
In the past antibiotics were often used as growth promoters; to increase the amount of meat rather than to treat illness in the livestock. Although the use of antibiotics as growth promoters is now banned in most countries, there is a concern that economic concerns could drive unscrupulous farming practices. Also even when farmers legitimately use antibiotics to treat infections in animals, they are often administered to the whole herd rather than targeted infected animals.
Whenever you take antibiotics either correctly or not, they ultimately end up in the environment. Studies have found antimicrobial resistance genes nearly everywhere we have looked, from nearly every Chinese River, to the remotest regions of the Amazon.